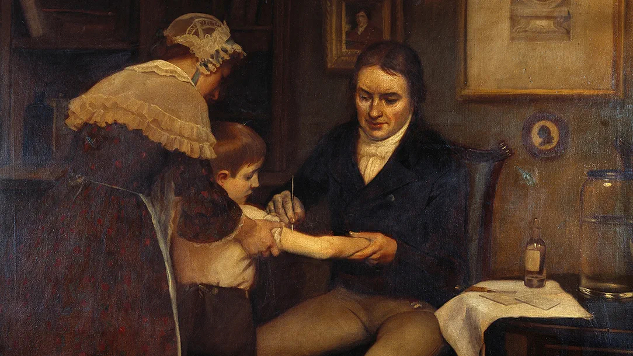
Vaccines are one of the few inventions in history that fundamentally shifted the balance between life and death. They turned once-feared killers into footnotes in medical textbooks. But in the United States, vaccine hesitancy is now threatening to undo decades of hard-won progress. What happens when a society forgets why it got safer in the first place? That question is no longer theoretical, it is the storm gathering on the horizon.
In This Article
- How have vaccine benefits reshaped public health?
- Why vaccine hesitancy is rising in the U.S.
- What economic savings vaccines deliver.
- Could preventable diseases return if rates drop?
- What America must do to protect progress.
Vaccine Benefits vs. Hesitancy: America’s Health at Risk
by Alex Jordan, InnerSelf.comStep back just one century. Smallpox still roamed the world. Measles was a childhood rite of passage, and polio stalked summer swimming pools. Families lived with an underlying terror: a child could wake up with a fever one day and never walk again. Vaccines erased much of that fear. They didn’t just reduce illness; they eliminated it in places that embraced immunization campaigns. Smallpox is gone. Polio, except in a handful of pockets, is nearly eradicated. These are not small victories, they are among humanity’s greatest triumphs.
Yet in the United States, the memory of those triumphs has faded. A younger generation, raised in an era when vaccines kept epidemics at bay, sees the act of vaccination less as liberation and more as intrusion. Ironically, vaccines worked so well that many now doubt they were ever needed in the first place. Comfort has bred amnesia, and amnesia has opened the door to doubt.
The Numbers That Matter
The Centers for Disease Control and Prevention recently calculated the impact of routine childhood immunizations since 1994. The results are staggering: over 1 million deaths prevented, 500 million illnesses avoided, and trillions of dollars saved. These aren’t abstract figures, they represent children who grew up, workers who stayed productive, and families spared from unbearable grief. In economic terms, vaccines have generated one of the highest returns on investment of any public health measure in U.S. history.
But numbers alone rarely shift opinion. The problem is not a lack of data; it is a lack of trust. And trust, once eroded, is harder to rebuild than it was to create in the first place.
Vaccine Hesitancy on the Rise
Vaccine hesitancy is not new, but its reach has widened. Fueled by misinformation, political polarization, and social media echo chambers, skepticism toward vaccines has gained traction in communities that once embraced them. The COVID-19 pandemic poured gasoline on this fire. Debates over mandates, personal liberty, and government overreach became proxies for deeper cultural divides. Vaccination, once a unifying act of collective protection, has been reframed as a partisan badge of identity.
When vaccination rates decline, diseases resurface. We are already seeing outbreaks of measles in parts of the U.S. that once had it eliminated. Whooping cough, long controlled, is creeping back. These diseases don’t politely wait for national debates to resolve themselves, they surge wherever immunity gaps appear.
The Economic Stakes
It is easy to think of vaccines purely in terms of lives saved, but their economic benefits are equally critical. Consider what happens when vaccination rates drop: hospitalizations rise, productivity falls, and healthcare costs balloon. An outbreak of measles in a single county can cost millions in containment, lost work hours, and hospital bills. Multiply that across states and years, and the hidden economic toll becomes immense.
The irony is that many who resist vaccination do so under the banner of financial freedom, resisting what they see as government interference, while the actual cost of hesitancy falls back on taxpayers, businesses, and communities. A society that refuses vaccines is not saving money; it is burning it.
History’s Hard Lessons
History offers a stark warning. In the early 20th century, when vaccines were still new, cities that embraced widespread immunization programs flourished with fewer epidemics. Those that resisted paid in lives and livelihoods. The 1918 influenza pandemic killed more Americans than World War I. By contrast, when polio vaccines were rolled out in the 1950s, communities embraced them eagerly, lining up at schools and churches to protect their children. The memory of iron lungs and summer quarantines made the choice obvious.
Today, many Americans do not carry those memories. Instead, they inherit a sanitized version of history in which deadly diseases are shadows, not present dangers. This generational amnesia weakens resilience against misinformation. If you’ve never seen a child paralyzed by polio, why fear its return?
The Cultural Divide
Vaccine hesitancy is not spread evenly across society. It maps onto cultural, political, and religious lines. In some conservative communities, distrust of federal agencies spills over into distrust of vaccines. In certain urban enclaves, alternative medicine subcultures feed skepticism. What unites these groups is not ideology but a shared suspicion of authority. When authority itself is discredited, even the most successful public health tools become targets.
This divide reveals a deeper problem: America’s fractured relationship with truth. Public health depends on shared facts and collective action. Vaccine hesitancy thrives in a culture where individualism is exalted above community responsibility and where misinformation spreads faster than correction. The fight over vaccines is less about medicine than about the kind of society America wants to be.
Consequences of Decline
If vaccine rates continue to fall, the consequences will not be abstract. Measles could reestablish itself as endemic, meaning outbreaks would no longer be rare events but regular cycles of disease. Whooping cough could surge, disproportionately harming infants. Polio, lurking in other parts of the world, could find footholds in under-immunized American communities.
Beyond health, the social consequences would be profound. Parents would once again fear sending their children to school during outbreaks. Employers would face increased absenteeism. Hospitals, already stretched thin, would buckle under preventable cases. The ripple effect would touch every layer of society, from education to commerce to national security.
What’s at Stake for America
At its core, the debate over vaccines is about whether America values collective security over individual suspicion. Vaccines are not just about the person receiving them, they are about the community that person lives in. Herd immunity protects the elderly, the immunocompromised, and infants too young to be vaccinated. To weaken vaccination rates is to weaken the shield protecting society’s most vulnerable.
This is not simply a medical debate; it is a moral one. Do we, as a nation, choose solidarity or isolation? Do we honor the legacy of science that lifted humanity out of the age of plagues, or do we risk tumbling back into it?
Rebuilding Trust
Solutions will not come from data alone. Trust must be rebuilt from the ground up. That means engaging local communities, empowering trusted messengers, and acknowledging legitimate fears without indulging falsehoods. Doctors, nurses, teachers, and even faith leaders must play roles. Public health campaigns must learn from the very forces that spread misinformation: storytelling, emotion, and repetition.
Most importantly, vaccination must be reframed not as an individual decision in isolation but as a shared investment in collective survival. Every shot in the arm is an act of solidarity, a recognition that health is not just personal but communal.
The Path Forward
The United States stands at a crossroads. On one path, it doubles down on science, trust, and collective responsibility, preserving the vaccine benefits that reshaped the modern world. On the other, it succumbs to vaccine hesitancy, inviting back the diseases our grandparents fought so hard to defeat. The choice may seem obvious, but history reminds us that civilizations often stumble not because they lacked knowledge, but because they lacked the will to use it.
What future will America choose? One built on the memory of progress, or one blinded by forgetfulness? The answer will not only shape health statistics; it will shape the very soul of the nation.
About the Author
Alex Jordan is a staff writer for InnerSelf.com
Recommended Books
The Vaccine Race: Science, Politics, and the Human Costs of Defeating Disease
A gripping account of the history of vaccines, this book explores the scientific breakthroughs, political battles, and ethical questions that shaped vaccine development in the 20th century. It is a reminder of both the promise and the price of progress.
Amazon: https://www.amazon.com/exec/obidos/ASIN/0525427538/?tag=innerselfcom
Vaccinated: One Man’s Quest to Defeat the World’s Deadliest Diseases
This biography of Maurice Hilleman, who developed over forty vaccines, illuminates the human effort behind one of the greatest medical revolutions. It offers both historical perspective and urgent relevance to today’s debates on vaccine hesitancy.
Amazon: https://www.amazon.com/exec/obidos/ASIN/B00E6T8YPY/?tag=innerselfcom
Deadly Choices: How the Anti-Vaccine Movement Threatens Us All
This book traces the rise of the modern anti-vaccine movement, showing how misinformation and cultural anxiety conspired to weaken public health. It offers a clear-eyed look at the consequences of choosing fear over science.
Amazon: https://www.amazon.com/exec/obidos/ASIN/0465057969/?tag=innerselfcom
Article Recap
Vaccine benefits have safeguarded millions of lives and strengthened the U.S. economy. Yet rising vaccine hesitancy threatens to reverse this progress. Understanding both vaccine benefits and the risks of hesitancy is vital for protecting America’s health, economy, and future.
#VaccineBenefits #VaccineHesitancy #PublicHealth #PreventableDiseases #HealthSecurity #Immunization #ScienceMatters